
How PANS/PANDAS Patients Can Change Brain Inflammation Research
A Conversation about the unhide® Platform I’m excited to share a recent conversation with Breanne Failor, Director of Strategic Partnerships at the Brain Inflammation Collaborative (BIC)....

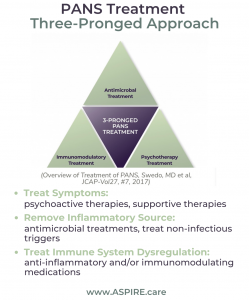



 PANS PANDAS Clinician Toolkit
PANS PANDAS Clinician Toolkit
 PANS PANDAS Guidelines for Children with Autism
PANS PANDAS Guidelines for Children with Autism











