
PANDAS is Autoimmune Encephalitis
"Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal infection or PANDAS can also be called post-streptococcal autoimmune basal ganglia...
PANS Consensus Statement on Diagnosing PANS and PANDAS –Clinical Evaluation of Youth with Pediatric Acute-Onset Neuropsychiatric Syndrome (PANS): Recommendations from the 2013 PANS Consensus Conference. Chang, MD et al (JCAP, Vol 25, No 1, 2015 Mary Ann Liebert, Inc.)
PANS PANDAS Symptoms PANS Consensus Statement
More on the PANS Diagnostic Process
The PANDAS Physicians Network (PPN) flowcharts for diagnosis and treatment will help clinicians evaluate their patients and determine the best course of treatment. Guidelines and workflows were approved by practitioners of the PANDAS Physicians Network Scientific Advisory Board. More detailed resources are available at www.pandasppn.org. Diagnosing and treating should be done by a licensed healthcare provider.
Primary care providers play important, ongoing roles in the diagnosis, treatment, and recovery of children with PANS/PANDAS. Children with a moderate or severe/life-threatening onset or a complex presentation may require treatment by an experienced multi-disciplinary team of specialists or a PANS/PANDAS specialist. Additional resources can be found at
PANS treatment utilizes three complementary modes of interventions to treat the patient completely. Three-pronged treatment protocols are dependent on disease trajectory, symptoms, and severity as well as lab work and patient history.
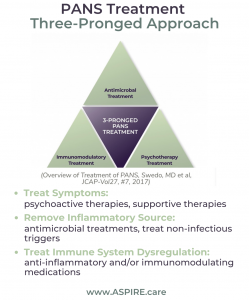
JCAP PANS Treatment Guidelines
The PANDAS Physicians Network (PPN) flowcharts for diagnosis and treatment will help clinicians evaluate their patients and determine the best course of treatment. The diagnostic flowchart and treatment guidelines include a detailed process provided for determining the appropriate diagnosis and symptom severity-based treatment protocols for mild, moderate, and severe/extreme cases.
Download PPN Treatment Flowchart
 PANS PANDAS Clinician Toolkit
PANS PANDAS Clinician ToolkitThere are invaluable resources to help clinicians learn how to recognize PANS PANDAS symptoms, do a workup to inform a possible diagnosis, and create a treatment plan. ASPIRE has assembled this one-page Clinician Toolkit but there are many resources throughout the website, and we are always adding more. So, check the website often.
 Diagnosis & Treatment of PANS PANDAS – Provider Packet
Diagnosis & Treatment of PANS PANDAS – Provider PacketClick the button below to download the twelve-page information packet Provider Information on PANS PANDAS, including Symptoms, Diagnosis, and Treatment.
 PANS PANDAS Guidelines for Children with Autism
PANS PANDAS Guidelines for Children with Autism
 Testing & Antibiotic Usage for GAS in PANS & PANDAS
Testing & Antibiotic Usage for GAS in PANS & PANDASASPIRE’S Professional Advisory Board Toolkit:
PANS is a clinical condition identified by an abrupt onset of a specific cluster of symptoms as a result of a variety of etiologies and disease mechanisms. Therefore, tracking symptoms, onset, severity, and duration is a critical part of making a clinical diagnosis and forming treatment plans. There are two useful PANS Symptom Rating Scale tools.

Developed by Tanya Murphy, MD and Gail Bernstein, MD. Source: PANS/PANDAS: CLINICAL & RESEARCH UPDATE, Gail A. Bernstein, M.D., 12/9/16, University of Minnesota
You can scroll through the pages of the Clinician Resources below. However, clicking on the link to the main Clinician Resources page is easier. Otherwise, you will be redirected to the top of this page each time you scroll to a secondary page in the resources.

"Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal infection or PANDAS can also be called post-streptococcal autoimmune basal ganglia...

This trifold brochure briefly explains PANS PANDAS, families' next steps, where to get more help and ASPIRE...

ASPIRE PANS PANDAS Current Resources for General Pediatricians. Share directly from this page or download it to email or print. Or contact us if you would like us to directly email your doctor or...

Overview – of PANS/PANDAS Symptoms, Diagnosis, and Treatment. For more in-depth information, please see the www.aspire.care website directly. Share directly from this page or download it to email...

There are invaluable resources to help clinicians learn how to recognize PANS PANDAS symptoms, do a workup to inform a possible diagnosis, and create a treatment plan. ASPIRE has assembled this...

The ASPIRE information packet on Advances in Research divides the research into sections in order to make it easy to review current research on a specific topic: JCAP diagnostic and treatment...

PANS PANDAS is medically complex. In order to have an informed discussion with your providers, it can be helpful to track symptoms, exposures to triggers, and medications. This Medication Log...

What is the relationship between PANS & PANDAS and Tourette Syndrome? Susan Swedo, MD and Gabriella True sit down to discuss the relationship between PANS & PANDAS and Tourette syndrome....

The Role of the Adaptive Immunity and Genetic Risk Factors in Vascular and Neuronal Dysfunction in Post-Infectious Autoimmune Encephalitis Available on Demand Presented by Dritan Agalliu, Ph.D....

“My Child Just Went Crazy One Day”: What You Need to Know about PANS & PANDAS, Ep. 125 CEU podcasts for social workers, psychologists, therapists, clinical counselors, and addiction...

Children brought to behavioral health clinics with a sudden onset of changes in behavior and/or mood are often misdiagnosed and mistreated because clinicians don’t know the signs and symptoms of...

At first glance, someone PANS and someone with OCD may appear pretty similar. They both have obsessions, compulsions, anxiety, and these symptoms cause significant distress, interfere with daily...