Repeated Flares & Baseline
Do patients go back to baseline between flares/exacerbations?
Not always. Some symptoms can remit fully while others are reduced but not back to baseline.
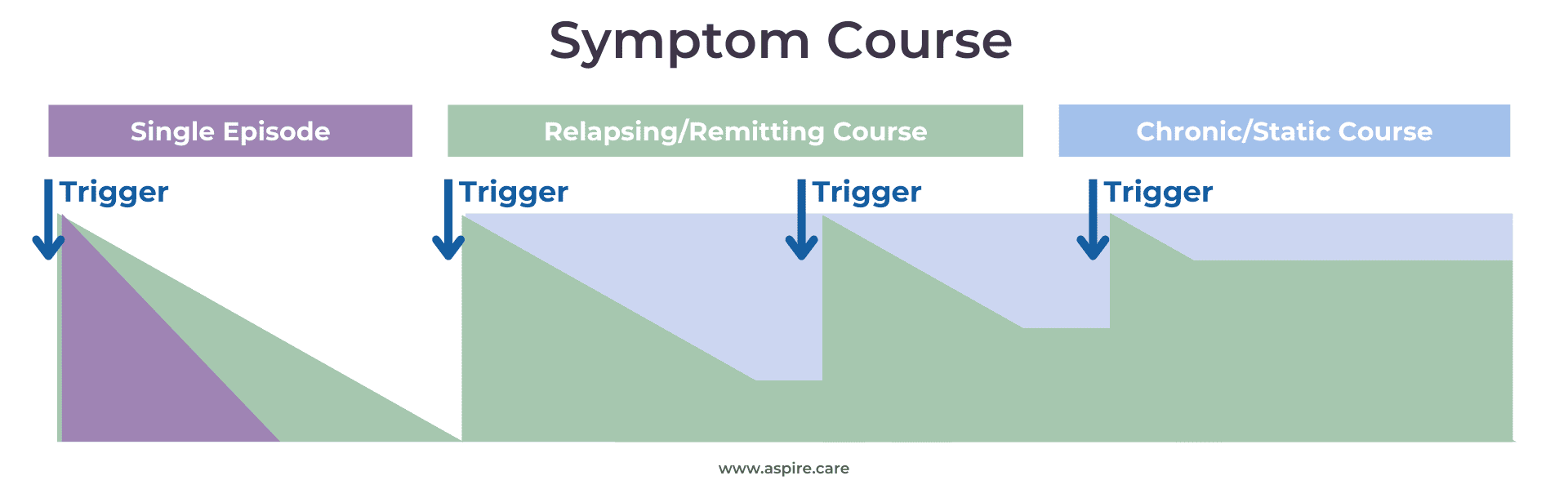 Note: PANS has multiple triggers, not just strep. This chart uses strep as an example incitatory trigger, but please note that any PANS trigger could replace strep on this chart. Learn more about the definition of PANS/PANDAS.
Note: PANS has multiple triggers, not just strep. This chart uses strep as an example incitatory trigger, but please note that any PANS trigger could replace strep on this chart. Learn more about the definition of PANS/PANDAS.
- The study standardizes definitions for PANS patient status and flares, including distinctions between flare and recovery, acuity of onset, duration, and symptom trajectory.
- 74% of patients meeting PANS criteria followed a relapsing–remitting course, rather than continuous illness
- 43% of patients experienced a persistent clinical course, defined as more than 12 months of functional impairment; however, 77% of these individuals ultimately recovered.
- 57% of patients did not develop persistent symptoms and typically experienced one to three flares per year, with each flare lasting approximately three months.
- These findings indicate that persistent symptoms do not preclude recovery, even following extended periods of impairment.
In clinical practice, some patients experience progressively severe or prolonged flares, with symptoms diverging further from baseline over time. When the majority of symptoms do not substantially remit between flares, the disease course may be classified as persistent or chronic. However, this classification does not eliminate the possibility of future improvement.
PANS symptoms can remit entirely, especially when identified and treated promptly and comprehensively. Treatment strategies should address both active flares and residual symptoms that have not returned to baseline, with the objective of restoring function and preventing chronic disability.
Relapses are frequently triggered by new infections, untreated or partially treated infections, environmental exposures, metabolic or inflammatory stressors, psychosocial stress, or physical injury. The severity of flares can vary considerably. Milder relapses should not be overlooked, as they may still indicate immune activation and contribute to cumulative impairment over time.
Learn more about PANS & PANDAS Symptoms
Learn more about PANS PANDAS Symptom Severity Differences